|
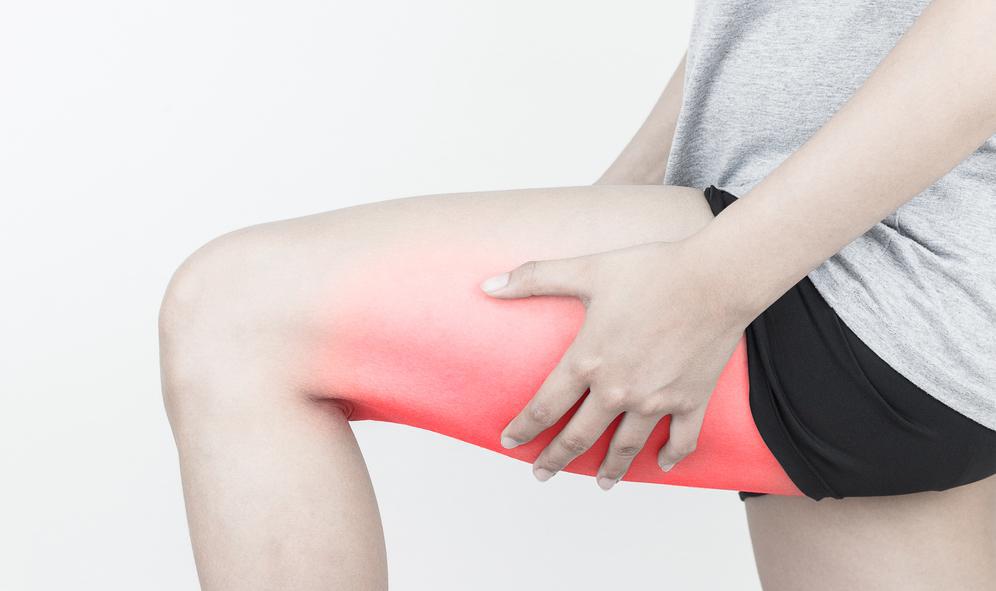
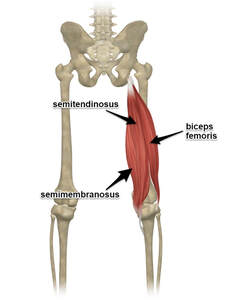
It is commonly believed that hamstring injuries cause the biggest time loss and are one of the biggest detrimental factors to team performance. This is in the elite sport setting but hamstring injuries are also very common in amateur and community sport as well. Hamstring injuries also don't have to be on the sporting field. One of the biggest risk factors for getting a hamstring injury is previous hamstring injury, so prevention is always better than trying to treat a previous hamstring injury. If you have been unfortunate enough to have had a hamstring injury, don't worry there are still things we can do to lower your risk. What are the hamstrings and what is a hamstring injury? The hamstrings are a group of muscles that sit at the back of your thigh. There are three, Bicep Femoris, Semitendinosus and Semimembranosus. All three cross over the hip and knee joints and therefore all three contribute to both hip and knee function. Their two primary roles are to flex or bend the knee and extend the hip. A hamstring injury is when there is a tearing of the hamstring muscle fibres because of an excessive force or stretching is placed upon the muscle fibres. Hamstring strains happen in all different activities but the most common way to injure a hamstring muscle is while running, and more specifically in the end of the swing phase of the running gait. During this phase the hip is going into flexion and the knee is going into extension. The role of the hamstring during this phase is to control these two movements and contract while lengthening, this is called an eccentric contraction and if there is too much force or the muscle is fatigued then a strain or a tear can occur. Acute rehab phase Directly after a hamstring strain it is important to use the acronym PEACE & LOVE (Protect, Elevate, Avoid anti-inflammatories, Compression, Education & Load, Optimism, Vascularisation, Exercise). Read our blog on this topic to learn more. Allowing the hamstring injury to recover by protecting it and not applying unnecessary excessive force initially and then also using movement and appropriate loading early in rehabilitation is the key for the best outcomes. Maintaining some form of exercise is also key, just because you have a hamstring strain does not mean you can't exercise. A great exercise for optimal loading is the Hamstring Isometric Holds, you apply isometric ( contraction with no muscle length change) loading to the muscle which can help with pain management and you can find the optimal load to apply which can be changed as you progress. Below is the hamstring Isometric holds. Try holding for up to 5 times for up to 30s. Getting back to activities Activities like walking and slow running are great exercises for improving the function of your hamstrings early on and should be a focus for hamstring rehabilitation after the initial acute phase. Building up hamstring strength in the gym or at home with exercises is also important to make sure the hamstring builds its capacity back to what it needs to tolerate to avoid another injury. In my personal opinion this step is probably the most skipped and could be a reason for some hamstring re injuries. What not to do Along with any injury rehab there are always things to avoid to get the best outcome and in hamstring injuries this is passive stretching! Passive stretching is forcefully putting the hamstring on stretch and holding this position and if you remember from my explanation above this is effectively putting the hamstring in the same position as how it got injured. Of course we want to maintain the length and function of the hamstring however passively stretching is not going to help this. What to do to maintain function and length of the hamstrings! Let’s let the powers of human function, biomechanics and brain power help us out. With every hamstring contraction there is another muscle on the front of the leg the quadriceps which is lengthening. If the quads activate then the hamstrings lengthen and the brain allows and facilitates this. So for an Exercise that helps with maintaining the function and length of the hamstring while injured try performing active knee extension and flexion either in lying or a seated position. Here shown in the lying position. Try it just gently to begin with. Going from injury to strength. In order to get the best possible outcome for your hamstring recovery it is important that you can progressively load and expose the hamstring to different types of stimulus. Probably the most important action for any hamstring recovery is trying to increase the maximal force that can be applied during an eccentric contraction, just like the mechanism of a hamstring injury. Mid to late stage exercises to perform to get back to activities effectively are shown below. I would also add getting back to high speed running progressively is also very important!
This type of bridge is best done in mid stage rehabilitation to build up the hamstrings tolerance for load. Begin with a double leg and progress to single leg.
* probably best done with a partner holding your legs but here I have used a heavy object on my heels.
The Nordic Hamstring Curls apply force to an eccentric contraction and help build up the strength in this particular movement. These exercises can be progressed and regressed according to how hard they feel, and should be done consistently after you return to your activity to help lower your risk of another injury. Keeping the hamstrings strong is pivotal in keeping you hamstring injury free. Of course this is not a complete guide nor is it a program to follow but it does give you an insight in how you can go from injury to strength. If you would like a personalised injury prevention program or a hamstring rehabilitation program contact the clinic. Izaac Boylan Accredited Exercise Physiologist
0 Comments
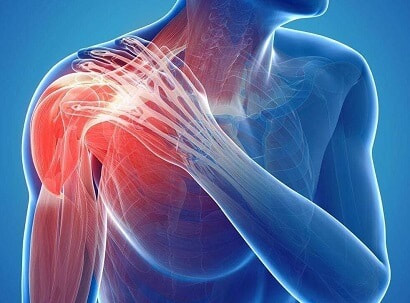
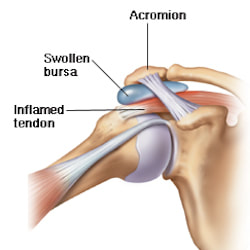
What is Bursitis? Bursitis is a condition that causes the small, fluid-filled sacs called bursae to become inflamed. A bursa is responsible for cushioning the tendons, ligaments, bones and muscles near the joint and preventing friction from occurring. This condition usually occurs in joints that are involved in repetitive movements, such as the shoulder, elbow, hip and knee. What are the symptoms? There are a range of symptoms that can present when bursitis has developed within the shoulder joint, including;
Causes of shoulder bursitis There are a number of potential causes but some of the most common can be a single injury such as a fall, repeated minor trauma like overuse injuries of the joint or muscles around the joint. When bursitis is caused from overuse injuries it is often associated with impingement and inflammation of the rotator cuff tendons as well. Prevention of shoulder bursitis Whilst it is difficult to determine singular causes in the development of bursitis there are a range of secondary factors that can contribute. Reducing causes of primary and secondary impingement are crucial in preventing shoulder bursitis and rotator cuff problems. Factors such as posture, muscle length, shoulder stability and rotator cuff strength can all contribute to the development of bursitis over time. Each of these factors can be optimised by completing specific exercises prescribed from a trained allied health professional. Treatment of shoulder bursitis
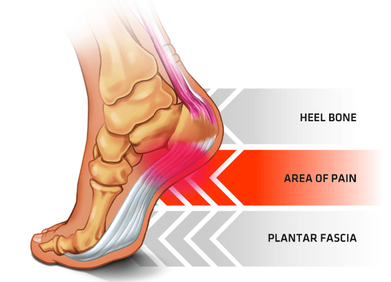
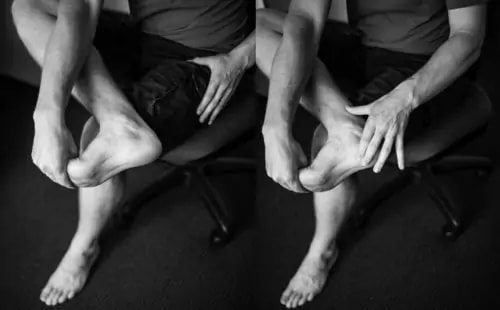
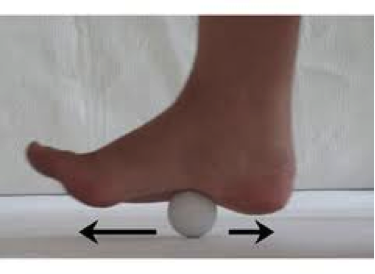
Shoulder bursitis is one of the most common shoulder injuries that presents in a range of populations. The rotator cuff muscles are responsible for the centralisation and stability of the shoulder joint. Adequate control within the shoulder then prevents injuries such as bursitis, impingement and dislocations. Interestingly, the arm only has one bony joint attachment where the collarbone meets the tip of the shoulder blade. The remainder of the shoulder joint attachment and stabilisers are all muscular, highlighting the importance of maintaining strength in the shoulder. Treatment for shoulder bursitis focuses on increasing range of movement in the shoulder joint without pain, regaining control of the shoulder blades, upper back and neck and improving strength in the rotator cuff and shoulder muscles. Each of these steps can take a number of weeks to successfully complete, so it is important to be patient and consistent during your treatment. If you suffer from shoulder bursitis, visit your local Accredited Exercise Physiologist who can help return your function and decrease pain! Written by, Aleisha Michael Accredited Exercise Physiologist. Plantar heel pain is something we see here in the clinic regularly and is something we have to be mindful of when prescribing exercise, particularly running or walking. Things that can increase your risk of plantar heel pain are overweight or obesity, a high increase in load such as running or walking and differing biomechanics of the leg and the foot (although this one is normally debated). What is plantar heel pain? Plantar heel pain is a term used to describe pain on the bottom of your foot near the heel. This umbrella term is sometimes used as it is debated as to whether the source of someone's foot pain can be determined. Terms like plantar fasciitis and plantar fasciopathy come under this umbrella term. Some experts use plantar heel pain prior to any ultrasound findings on the plantar fascia and before they can confidently diagnose plantar fasciopathy. Plantar fasciopathy is due to degeneration resulting from micro tears and necrosis of the plantar fascia through overuse and unsuitable loading. Unsuitable loading of the plantar fascia means the demand on the tissue structure from an activity or from increase in weight is larger than the plantar fascia can handle. Treatments There is a wide variety of treatments for plantar heel pain with a varying degree of positive effects. Some opt for more passive treatments like heel inserts, rest, ice and taping while others try and use more active strategies like activity modification, stretching and strengthening. The good thing about treatments for plantar heel pain is that many out perform a placebo or no treatment at all meaning that by doing something is beneficial. But what is the best? If something hurts then rest it right? Well unfortunately although this will give you some pain relief, this will not prevent any further pain in the future when you return to your activity. Rest may be required initially for pain relief but gradual activity modification (instead of complete rest) and optimal loading to improve the plantar fascia’s durability is going to be best for long term solutions. What does the research say It is widely known that stretching is one of the most beneficial treatments for plantar heel pain out there. Now however there is more evidence to suggest adding high slow resistance training can improve recovery even more. Advice and patient education is also key to helping people recover from plantar heel pain. Advice for people living with plantar heel pain (picture adopted from Dr Michael Rathleff research) If you have plantar heel pain and want to do something about it here are 3 strategies to try. Stretching (picture adopted from Dr Michael Rathleff research) Stretching prescribed here at the clinic is something that has been researched and proven effective. As seen in the picture above, grasp at the bottom of the toes on the bottom of the foot and pull your toes towards your shin bone until you can feel a stretch in the arch of your foot. Try this method 10 times for 10 seconds and try it 3 times a day. Rolling on a ball Using a similar mechanical method as stretching, rolling on a ball of any kind has been seen to have some positive benefits. Simply roll bare feet on a ball through the arch of your foot. The ball does not have to be a specific type of ball, any little ball will have an effect eg. cricket ball, golf ball and even a tennis ball. Try 5 times for 1 minute and try it 3 times a day Heavy Slow Resistance Training Strengthening has been proven to show significantly improved outcomes after the 3 month mark of rehabilitation compared to stretching. Here is how you would do it. As seen in the Video, use a towel so your toes are in a fully extended position on a step. Then perform a double leg or single leg calf raise slowly. It should take you 3 seconds to get to the top of the calf raise, staying for 2 seconds at the top and 3 seconds to return back down. Performing slowly will help to reduce any flair ups and increase time under tension. Try this exercise 12 reps x 3 sets with a weight you feel you could not lift any more than 12 times. Using books in a backpack is a good way to add weight. Single leg will be harder then double leg. When you feel you are getting stronger, Add more weight. An accessible level of pain to you is okay, however if your symptoms increase during the exercise or the next day, the load is too high. There is a quick review of what to do if you have plantar heel pain. It is only a guide and should not be taken as specific advice for you. If it is something you really want to get on top of, see one of our exercise physiologists. Izaac Boylan Accredited Exercise Physiologist So, you work in a physically demanding job and feel that this gets you enough physical activity throughout your day that you don’t need to do any extra, right?... WRONG. Whilst all this extra incidental activity throughout your day is giving you additional health benefits, it doesn’t give you the same BENEFITS as structured physical activity. What is the difference between incidental and structured physical activity? Incidental activity is defined as NON-PLANNED, UNSTRUCTURED ACTIVITY that accumulates in small portions over the course of a day. It can take many different forms including;
Whereas structured physical activity is PLANNED ACTIVITY that is completed in a continuous bout. This includes a planned walk, run or bike ride, gym sessions or classes or any other planned exercise session done individually or with others. Can I just do incidental activity? Whilst incidental activity provides many positive benefits it does not provide the same degree of benefit as structured physical activity. This is due to structured activity being completed in a continuous bout enabling our heart rate to increase, improving our cardiovascular and respiratory health. Completing specific strength training in planned exercise sessions also promotes a further increase in muscular strength and endurance when compared to incidental activity. Research has also shown that when activity is completed at a moderate intensity it assists in the prevention of a number of chronic conditions, including but not limited too;
What are the benefits of incidental activity?
By keeping your daily routine as active as possible there are a number of benefits that occur as well, such as;
So, what type of activity should I focus on? At the end of the day all movement counts and should be encouraged, whether it is a planned workout or sneaking a few extra steps in around the office! If you feel that you have been lacking with your structured physical activity recently, try adding in a few extra steps to your day by parking the car further away, taking the stairs instead of the lift or getting up from your chair once every hour! If you would like some more guidance about how to fit structured or incidental activity into your day try visiting an Accredited Exercise Physiologist! By, Aleisha Michael Accredited Exercise Physiologist. Christmas has come around again. It is the time of year where we might over indulge on christmas food or we use this time for a little bit of rest and relaxation and sometimes we may forget to move or do some exercise. Exercise is something that can be hard to commit to while in relaxation mode but it is very important to continue while you are on holiday. As we have said before exercise is a vital part in your wellbeing and keeping up your exercise routine will help you to relax and recharge ready for the new year! Although keeping up a similar exercise routine is the best way to go, it may not be possible depending on your holiday plans. If you are away from home and can't continue what you have been doing throughout the year, I will provide you with my top 5 exercises that can be done without any equipment and can be done from anywhere. Bird dog The bird dog is a great exercise for hip, shoulder and core stability. It is easy to perform, can be performed in a variety of settings and has some variations that might make it a bit more simple for you to start with. To perform:
The video below will demonstrate Push ups The push is an easy to perform and well known exercise that can be also done with many variations. The push up is great for general upper body strength and has some element of core stability as well. To perform:
The video below will demonstrate. Squats Again, the squat is a very common and well known exercise and believe it or not we do some form of a squat throughout each and every day. An excellent exercise for lower body strength and a fundamental movement. To perform:
The video below will demonstrate. Deadbugs The deadbug is a great exercise for core strength and can be done anywhere there is free space on the ground or in a bed. It is a similar exercise to the bird dog, just upside down! To perform:
The video below will demonstrate. Lunges Another great exercise for lower limb strength and something that can be done again with no equipment To perform:
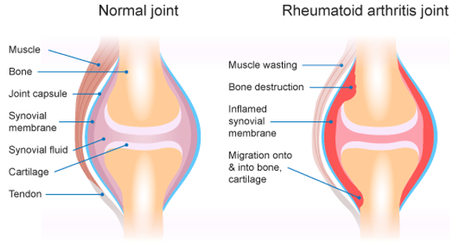
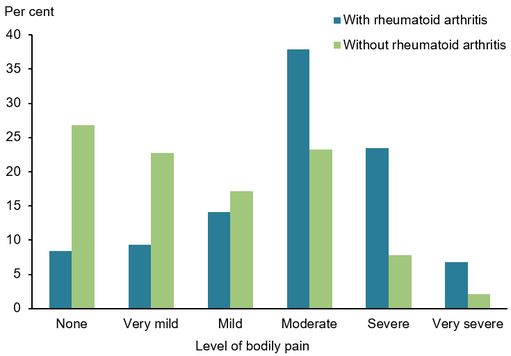
The video below will demonstrate. Bonus Exercise - Walking Walking is the simplest form of exercise, done with no equipment, can be done anywhere, and really can be done anytime. Walking has multiple benefits for your psychological and physical well being and can be tailored to your ability by changing time, distance and/or pace or intensity of your walking. I recommend trying to walk every day for at least 30 mins throughout the holiday period and beyond. Well there you go, 5 easy to perform exercises that will help you maintain some strength throughout the holiday period and beyond! Remember if you need specific advice contact the clinic in the new year and we can start your exercise journey the right way! Merry Christmas & Happy New Year! Izaac Boylan Accredited Exercise Physiologist What is Rheumatoid Arthritis? Rheumatoid Arthritis (RA) is an inflammatory autoimmune disease that occurs when our immune system begins to attack its own tissue. It usually targets joints and specifically the very thin, smooth membrane that lines the joint, providing it with lubrication and nourishment. When this happens, the joint lining (otherwise known as the Synovial Membrane) can become thickened and inflamed causing potential bone erosion or growths to form. In this picture we can compare a healthy ‘normal’ joint on the left with a think layer of synovial fluid and synovial membrane surrounding the cartilage and bone, protecting the joint. In comparison on the right, we have a joint suffering from RA, with a significantly inflamed synovial membrane that is radiating into the surrounding bone and cartilage. Am I the only one suffering? You are not alone if you have been diagnosed with RA, as over 456,000 people in Australia have reported having RA and it being 1.5 times more prevalent in Women compared to Men. Data has revealed that the initial onset of RA happens most commonly between the ages of 35-64 and those over 75 years old having the highest reported incidences of RA. A study conducted by the Australian Institute of Health and Welfare that compared bodily pain levels in those with and without RA reported that in participants with RA, aged 45 and over, 68% experienced ‘moderate’ to ‘very severe pain’ in the 4-week study. This made those with RA 3.1 times more likely to experience pain classed as ‘severe’ or ‘very severe’ when compared to those without the condition What can I do to ease the pain? The good news is RA pain levels and flare ups can be significantly reduced through REGULAR AND EXPERTLY PRESCRIBED EXERCISE. We understand that it can cause anxiety and worry when exercising with RA, in fear of increasing pain within the inflamed joints BUT, research tells us that exercise is a crucial element in managing pain and flare ups. We know that movement assists in DECREASING STIFFNESS AND INFLAMMATION as it increases lubrication within the joint. Decreasing the level of stiffness within the joint will also INCREASE ITS RANGE OF MOVEMENT, providing a prolonged improvement in mobility. Regular strengthening exercise will also increase the strength of those muscles surrounding the affected joint, REDUCING THE LOAD AND IMPACT they are required to endure. As WEIGHT LOSS can be a by-product of regular exercise this can also assist in reducing the load placed on the joint, decreasing inflammation and wear and tear. Not only will regular exercise reduce your RA flare ups and pain levels, it also PROVIDES ENDLESS BENEFITS TO YOUR PHYSICAL AND MENTAL HEALTH long term. This can include preventing the onset of other co-morbidities like heart disease, lifestyle-based diabetes, obesity and even other forms of arthritis. It also improves your mental health, mood, motivation and energy levels to help get you back to doing the things that you enjoy most. Should I exercise during a flare up?
The research states that during a flare up the best practice is to rest the affected joint and COMPLETE LIGHT RANGE OF MOVEMENT BASED EXERCISES, to prevent prolonged stiffness building up within the joint. These movements should be done several times per day and pushed as far as is comfortable. Whilst gentle movements will help to reduce the overall flare up time, resistance and wights should not be used during these periods. So, what types of exercises are best? There is no one size fits all exercise program for those with Rheumatoid Arthritis and programs should be individualised and tailored to you are your specific presentation. BUT.. the best type of exercise is the one that you enjoy doing the most, as this increases your likelihood to engage in it long term. In regards to assisting with RA pain and flare ups, generally low impact movements are best suited to prevent aggravating the joint. There are 3 main goals involved in RA based exercise programs;
By Aleisha Michael, Accredited Exercise Physiologist. Injuries are a very common occurrence in sport or the workplace and there are a multitude of factors that play a role for an injury to occur. Injuries can be niggling and can threaten to derail your sports season. Injuries also play a role when it comes to limiting you at work and your everyday life and therefore I feel injuries are very important to manage correctly. Below will outline what the most recent and up to date research says about how you should go about your rehabilitation so you can recover in the quickest time possible with the best outcomes possible. Have you heard of RICE ( Rest, Ice, Compression and Elevation)? Or what about POLICE ( Protection, Optimal Loading, Ice, Compression, Elevation)? These 2 acronyms have been used throughout the years as ways to help people manage injuries and at the time were based on the latest research. These practices are still very commonly used when someone suffers an injury. But is this what the latest research says? Are we providing the best management for our injuries? In 2019 new research emerged and with it, a new acronym for us to live by when managing injuries, PEACE & LOVE. This new acronym helps us manage directly after an injury has occurred, but also gives us a framework for management to get back to pre-injury capacity. What does this mean for us who are trying to manage an injury? Well I will go through step by step. The word PEACE helps us understand what the necessary approach is directly after an injury has occurred. P for protection It is recommended to minimise movement and load on an injury for the first 1-3 days to reduce the risk of aggravating the injury, minimise bleeding to the area and prevent distension to the injured muscle. E for elevate Elevate the limb or body part higher than the heart to be able to remove any unwanted fluid around the injury. A for avoid anti-inflammatories The body’s way of repairing an injury is through inflammation. Inflammation carries all the right things for your body to go through the process of repairing itself. Therefore taking anti-inflammatories which are designed to stop this process could affect long term healing. What about ICE? It has been a stalwart in the injury management space for many years now but according to the most recent research it is unknown whether ice helps the healing process of an injury. It is believed ice reduces inflammation which we know is very beneficial and necessary to healing. In fact the researcher, by the name of Dr Gabe Mirkin, who invented the term RICE back in 1978, has retracted his research and now has the view that ice and rest may actually delay healing not help it. Ice is thought to have a pain relieving effect on an injury and therefore does have a role in injury management but not as initially first thought. C for compression Compressing an injury with external pressure like a bandage or compression garments you can buy these days assists to reduce swelling and muscle bleeding E for education Correct education from a health professional helps to avoid overtreatment and should give you the confidence in your body’s healing mechanism. You should be trying to stay away from passive treatments especially in the long term and try to use more active approaches to management. The mentality “I need fixing” is detrimental to your recovery. If you don't understand your specific injury or don't know how to rehabilitate it, speak to a health professional for help and education on correct treatment and load management for a full recovery. & After the initial management of an injury, all it needs is some LOVE. L for load Load should be added early on in your rehabilitation and you should try and resume your normal activities as soon as you feel comfortable doing so. Loading that does not exacerbate pain assists repair and recovery of your muscles, allowing you to regain the capacity and strength you previously had. O for optimism Psychological factors play a larger role in a person's recovery than people release. Factors such as catastrophizing your injury and fear or anxiety over your injury can prevent optimal outcomes. It is believed that psychological factors may drive the variation you see in certain injuries, more so than the injury itself. Stay positive, be optimistic and believe in your body’s healing process. V for vascularisation Aerobic exercise is a fundamental aspect of any injury rehabilitation process as it promotes blood flow to the injured area and is proven to improve mood, psychological well being and motivation. So find a pain free aerobic exercise that you enjoy and begin with that. E for exercise
Exercise is thought to be the gold standard in terms of treatment for injuries and research has demonstrated positive outcomes for all types of injuries. Exercise has many different mechanisms of improving the capacity of an injured body part or an injured person and it is important to continue to exercise any way possible through an injury period. There is plenty to understand and to cover when you get an acute injury however remember to use the acronym PEACE for directly after an injury has occurred and use love for the rehabilitation process. Bottom line is you want to stay as active as you can and in the beginning phase of an injury be guided by your pain to what you can and can't do. Loading the injury to a tolerable level is only helping healing, not hindering it. Izaac Boylan Accredited exercise physiologist 1. Strength Training improves muscle mass, which can help us in our everyday lives Looking like the incredible hulk or the next bodybuilding queen are not the only reasons to strength train, and for probably around 98% of the population, these are not the reasons we strength train. Some might strength train to improve their athletic performance, improve flexibility and reduce incidence of injury or chronic disease. However, at the very least improving your strength can help with everyday tasks such as moving the lawn, lifting the groceries, shifting furniture, and cleaning your house. For most people these jobs are not the most enjoyable in the world, therefore having good strength and stamina to get them done quicker and with less effort is a great outcome. 2. Strength training improves bone mineral density As we age, and particularly for females who are post menopausal, our bone mineral density can decline. There is evidence to suggest that we can lose as much as 3-5% per decade after the age of 30. This can increase a person's risk of a fracture if they were to have a fall, and lead to reduced quality of life. In a study of people living with Osteoporosis who undertook a specific strength training program to improve bone density, results showed that 86% of patients increased bone mass in their lower spine, and 69% of patients increased their bone mass in their hip - which is great results for people living with this condition. 3. Strength training can help to preserve lean muscle mass during weight loss Generally when you restrict our energy intake with the goal of losing weight, not only do you lose fat mass, but also some lean muscle mass, which is not ideal. Although aerobic exercise generally forms the basis of your training if your goal is to lose weight as this form of exercise burns a greater amount of energy during your exercise session compared with strength training. Strength training does help you to maintain and preserve your muscle mass during weight loss, and can increase your excess post-exercise oxygen consumption, meaning your metabolism remains active and your body continues to burn calories after you have completed your workout. Therefore, adding resistance/strength training exercise on top of your aerobic training is beneficial when losing weight. 4. Strength training can improve your flexibility When most people consider improving their flexibility, usually yoga, or undertaking specific static stretching exercises comes to mind. Both of these activities are effective in improving the flexibility of a joint, however undertaking full range strength training has also been shown to be just as effective as flexibility training for a specific joint, and not surprisingly both are superior to doing nothing (reference). Therefore, adapting your program to include some full joint strength exercises can effectively kill 2 birds with one stone, and reduce the need for a specific flexibility program for those strength trained joints.
Lisa Parkinson
Accredited Exercise Physiologist & Credentialed Diabetes Educator 1. Check what you are drinking
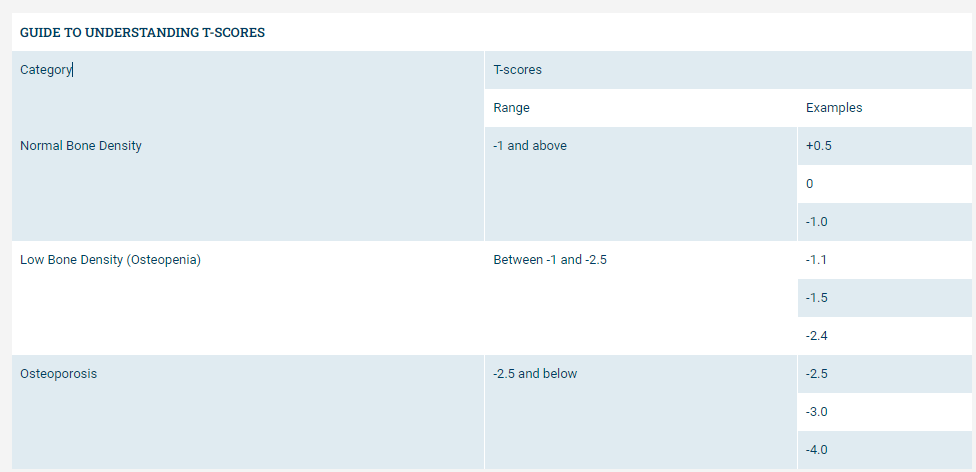
Many people know they need to watch what they eat, but what about what you are drinking? There may be loads of hidden sugar in lots of drinks that you are not aware of. For instance a 250ml glass of wine has about half a teaspoon of sugar; a glass of OJ or cordial contains about 6 teaspoons of sugar; and a can of coke contains around 9 teaspoons of sugar. One way to reduce the amount of sugar and energy you are consuming during the day is by reducing these sweet drinks, and reaching for our water bottles. 2. Increase your NEAT exercise NEAT stands for Non Exercise Activity Thermogenesis. Basically this is the energy that we burn when we are undertaking any activity that is not considered to be exercise. So .... taking the stairs rather than the lift, parking the car further away, walking to work, etc are all increasing our NEAT. This is a really neat way to increase the amount of energy we burn throughout the day without actually undertaking any planned activities. However, planned activities are also essential for our health and well-bing. 3. Check your portions Maintaining a healthy weight is not just about what you eat, but how much you eat; and too much of a good thing isn’t always a good thing! Meat is one area, that particularly men, tend to overeat. It is recommended that men between the age of 51 and 70 limit themselves to 2.5 serves of lean meat each day. A serving size of cooked lean meat for a male aged 51-70 is 65g, that’s no more than the size of your palm. If you are eating poultry it is 80 grams and 100g for seafood. Many men eat double this at dinner, let alone adding in what they also have for lunch, and other protein sources such as eggs and nuts. 4. Take a walk after dinner Our blood glucose levels generally peak about 2 to 3 hours after we eat. For those people who have pre-diabetes or type 2 diabetes, exercise helps to use the glucose in our blood without the use of the hormone insulin. And this is a great thing for our bodies because exercise can help to reduce our blood glucose levels post meal, therefore decreasing the demand on pancreas to do the job all by itself. The effects that exercise has on improving this process, lasts up to 72 hours post exercise session. A great reason to exercise at any time, but it is also really useful after a big meal. 5. Get a good night’s sleep Sleep may be just as important as eating healthy and exercising. Studies show that poor sleep is one of the strongest risk factors for obesity, as it’s linked to an 89% increased risk of obesity in children and 55% in adults. However the good news is that there does appear to be a positive influence of exercise on sleep disorders. Quality of life and/or severity of sleep disorders appear to be positively impacted by regular exercise. Adopting a physically active lifestyle may be a key intervention for the treatment of sleep disturbance and obesity, and may be a long-term solution to improved quality of life and decreased risk for the chronic conditions associated with these Sleep disorders. Lisa Parkinson Accredited Exercise Physiologist & Credentialed Diabetes Educator What is Bone Mineral Density and how does it cause Osteoporosis? Bone Mineral Density (BMD) refers to the amount of bone mineral in bone tissue. When experiencing Osteoporosis or Osteopenia BMD can decrease, placing individuals at a higher risk of fractures or breaks in bone. Osteoporosis is more common in post-menopausal women as their BMD levels continue to decline with age. BMD levels have shown to be lowest in the spine and the neck of the femur (thigh bone), and these are 2 of the sites tested when you have a bone mineral density scan. When you have a BMD scan, you will be provided with a T-score for each of the bone sites tested. This T score is compared to the T-score of a healthy 30 year old, and gives and indication of how high or low your bone density is. The table below shows the T-scores and their classifications for normal bone density, osteopenia, and osteoporosis. How can I improve my bone mineral density? There are a few different methods in which your BMD can be increased;
How can exercise make my bones stronger? Studies have shown that therapeutic based exercises that include resistance and load bearing movements are able to MAINTAIN OR IMPROVE BONE MINERAL DENSITY LEVELS in healthy individuals and those diagnosed with Osteoporosis. These exercises have been reported to STIMULATE BONE GROWTH AND PRESERVE BONE MASS. These processes occur through a mechanical stimulus on the bone and both anti-gravity loading, and stress exerted on the muscles that surround it. Quite simply, this means that movements involving repetitive and loaded (heavy) exercises cause the working muscles involved to pull on the bones they are attached to, which in turn stimulates bone growth. When this is completed on a regular basis over a long period of time it can have a significant effect on BMD levels. What type of exercise is best? There has been a large amount of research conducted into which exercise type provides the best results when trying to increase bone mineral density. The Onero program has collated and completed multiple studies to determine which exercise type reigns supreme and designed a program to specifically include these exercises. They research found that IMPACT AND RESISTANCE-BASED TRAINING THAT IS BOTH SUPERVISED AND TARGETED provides the highest improvement in BMD. The Onero program ongoing data has shown that 86% of participant’s had an increase in lumbar spine (LS) BMD, whilst 69% had an improvement in femur BMD. Results have also shown a significant improvement in participant’s posture and a decrease in falls risk, preventing potential fractures. Overall, high intensity loading and impact-based exercise undertaken in a safe and supervised setting are the most optimal types of exercise to increase BMD. These exercises are an example, however all exercises are safely prescribed for the individual at the entry level appropriate for their health, conditions, fitness and confidence. Who can help me increase my Bone Mineral Density safely? Accredited Exercise Physiologists are the most appropriate people to assist you in increasing your BMD. The great news is that Optimum Exercise Physiology, runs a Strong Bones specific class twice a week that has TAILORED AND SPECIFIC EXERCISE PROGRAMS THAT ARE SUITABLE TO YOUR CURRENT NEEDS AND GOALS. Can't make a class, that's fine too. We can develop a program for you to undertake independently at the gym or for home. Would you like more information ...?
If you would like more information about how exercise can help improve your bone mineral density and reduce the risk of developing or progressing Osteoporosis/ Osteopenia further, please get in touch on 8873 0628 or, info@optimumep.com.au. By, Aleisha Michael, Accredited Exercise Physiologist. |
AuthorSLisa Parkinson Archives
March 2024
Categories
All
|











 RSS Feed
RSS Feed