|
So, you work in a physically demanding job and feel that this gets you enough physical activity throughout your day that you don’t need to do any extra, right?... WRONG. Whilst all this extra incidental activity throughout your day is giving you additional health benefits, it doesn’t give you the same BENEFITS as structured physical activity. What is the difference between incidental and structured physical activity? Incidental activity is defined as NON-PLANNED, UNSTRUCTURED ACTIVITY that accumulates in small portions over the course of a day. It can take many different forms including;
Whereas structured physical activity is PLANNED ACTIVITY that is completed in a continuous bout. This includes a planned walk, run or bike ride, gym sessions or classes or any other planned exercise session done individually or with others. Can I just do incidental activity? Whilst incidental activity provides many positive benefits it does not provide the same degree of benefit as structured physical activity. This is due to structured activity being completed in a continuous bout enabling our heart rate to increase, improving our cardiovascular and respiratory health. Completing specific strength training in planned exercise sessions also promotes a further increase in muscular strength and endurance when compared to incidental activity. Research has also shown that when activity is completed at a moderate intensity it assists in the prevention of a number of chronic conditions, including but not limited too;
What are the benefits of incidental activity?
By keeping your daily routine as active as possible there are a number of benefits that occur as well, such as;
So, what type of activity should I focus on? At the end of the day all movement counts and should be encouraged, whether it is a planned workout or sneaking a few extra steps in around the office! If you feel that you have been lacking with your structured physical activity recently, try adding in a few extra steps to your day by parking the car further away, taking the stairs instead of the lift or getting up from your chair once every hour! If you would like some more guidance about how to fit structured or incidental activity into your day try visiting an Accredited Exercise Physiologist! By, Aleisha Michael Accredited Exercise Physiologist.
0 Comments
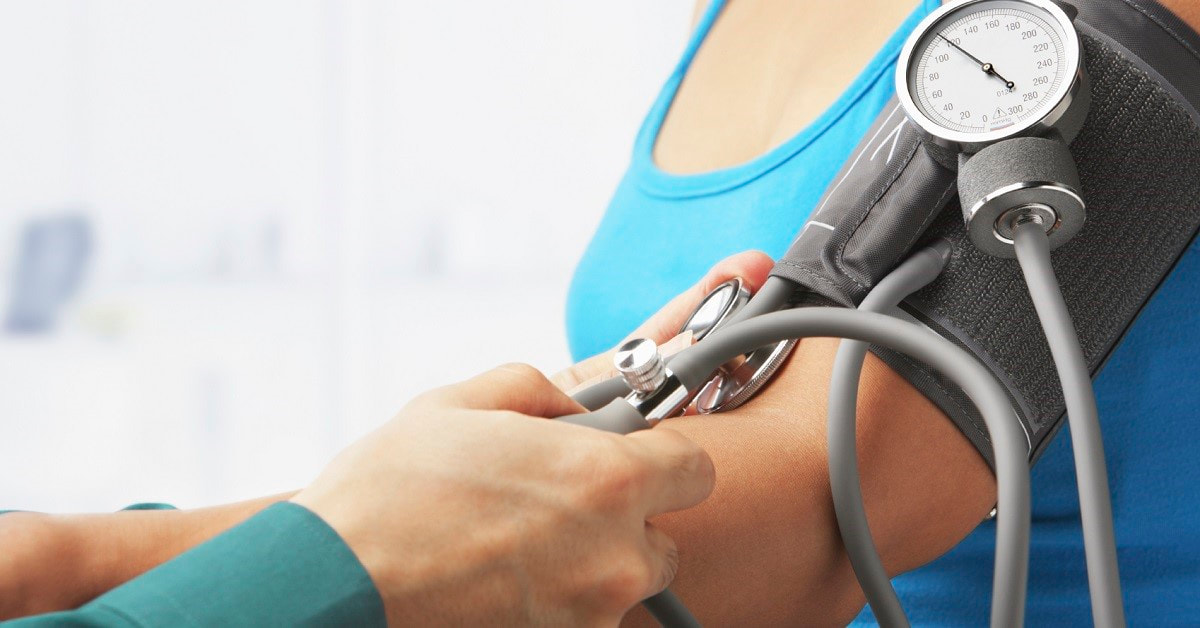 Have you recently been told you have high blood pressure or hypertension? Are you sick of taking medications every day to help manage your high blood pressure? Are you concerned about your high blood pressure putting you at an increased risk of cardiovascular diseases like heart attacks and stroke? Then it might be time for you to get moving! What is hypertension? Hypertension or high blood pressure occurs when the pressure of your blood against the walls of your blood vessels is too high for a prolonged period of time. This pressure is created when your heart beats and is the result of two forces. The first force is your systolic pressure which happens when blood is pumped out of the heart to the rest of the body. The second force is your diastolic pressure, and this occurs when the heart rests between two beats. One of the main reasons that high blood pressure can cause harm is that the constant increase in workload and pressure makes the heart and blood vessels work harder and less efficiently. This can eventually cause damage to the internal tissues, tiny tears in the artery walls, and plaque entering these tears and causing narrowed blood vessels, which further increases your blood pressure. How does exercise help? I’m sure that we are all aware that movement in any form is good for our bodies, but the question is how is it helping our blood pressure specifically? There is a lot of research supporting the benefits of exercise and evidence proving that regular physical activity and moderate levels of cardiovascular fitness protect against the development of hypertension and all cause mortality. Regular aerobic exercise has been proven to decrease daytime blood pressure readings of both the systolic and diastolic values. This decrease occurs because the heart is a muscle and when we exercise this muscle is worked and becomes stronger as a result. When the heart is stronger it is able to pump more blood around the body with less effort, which as a direct result lowers the pressure that is being put on your arteries with every pump. How much exercise should I do? The National Heart Foundation of Australia provides recommendations around physical activity to help manage a healthy blood pressure. We should be engaging 150-300 minutes of moderate intensity activity or 75-150 minutes of vigorous intensity exercise each week. Individuals should also be completing muscle strengthening activities on at least 2 days of the week. Initially this may sound like a lot but it’s as simple as a 30-minute walk 5 days per week and lifting something heavy two days a week. Or if you’d rather smash it out in fewer days, try a 45-60-minute walk 3 days a week and lifting something heavy for 2 days. Before you get started..
By Aleisha Michael Accredited Exercise Physiologist 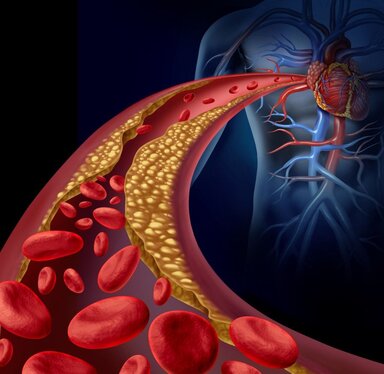 Dyslipidaemia refers to abnormal levels of blood fats or ‘lipoproteins’. Lipoproteins are the transporters that move fat around our bodies. The most common dyslipidaemias are high blood cholesterol and triglyceride levels known as hyperlipidaemia, high levels of low-density lipoprotein cholesterol (LDL-c, the ‘bad’ cholesterol) and low levels of high-density lipoprotein cholesterol (HDL-c, the ‘good’ cholesterol). How is it diagnosed? A blood test called a lipid profile is used to diagnose the condition, and management of dyslipidaemia is important for people with, or at risk of, cardiovascular disease because we know that a poor lipid profile is a significant risk factor for blood vessel damage. The risk of heart problems also increases with high triglyceride or LDL-c levels, or with low HDL-c levels. How does exercise help? Management of dyslipidaemia aims to reduce the risk of cardiovascular ‘events’ such as heart attacks that may occur within the next 5-10 years — this is called the absolute cardiovascular risk. Any lowering of LDL-c and triglycerides, or raising of HDL-c, is likely to reduce this risk. Improving our lifestyle by improving our diet, increasing our exercise to reduce our weight, especially body fat, is a key management strategy for decreasing cardiovascular risk. Physical fitness and regular exercise have both been shown to considerably reduce the absolute cardiovascular risk and death rate. Studies have shown that regular aerobic exercise can:
What types and intensities of exercise are recommended? People with dyslipidaemia should undertake aerobic exercise for at least 30 minutes on most, if not all, days of the week to improve their lipid profiles and reduce their cardiovascular risk. This amount can be accumulated in shorter bouts of 10 minutes duration and can be built up over time. We suggest aerobic exercise that uses large muscle groups such as brisk walking, jogging, cycling, swimming, dancing, skiing, playing ball games or other sporting activities. Research has also found vigorous aerobic exercise to be beneficial and improves HDL-c more than less-intense exercise. Vigorous aerobic exercise is described as a ‘very hard’ effort, and at this level you would not be able to hold a conversation whilst exercising as you would not have the breath to do so. In addition to aerobic training, progressive high-intensity resistance training (i.e. weight training) has also shown to improve HDL-c. For this the goal is to undertake 2–3 sets of 8–10 different exercises, at a load that can be performed for 8–15 repetitions of each exercise, at least twice a week. Don’t forget your warm up before both your aerobic and strength training exercises. Precautions People with known or suspected cardiovascular disease, metabolic syndrome or diabetes; people with a family history of heart attacks; people with high blood pressure; smokers; men aged over 45 years or women aged over 55 years; and people who have not been doing regular exercise should consult their doctor or Exercise Physiologist before commencing an exercise program. Lisa Parkinson Accredited Exercise Physiologist |
AuthorSLisa Parkinson Archives
July 2024
Categories
All
|



 RSS Feed
RSS Feed