|
What is diabetes? Diabetes is a chronic health condition which occurs when there is too much glucose within the blood. Either the body is unable to make insulin, make enough insulin or the body is unable to effectively use the insulin that it does make to lower or maintain our blood glucose levels within normal readings. The three different types of diabetes include type II, type I and gestational. It is currently estimated that more than 415 million individuals around the world have diabetes, with >90% of these individuals having type II. Staggeringly, this number is expected to increase by more than 50% by 2040. However, fortunately research has demonstrated that exercise can be used as an effective tool to assist with the management of diabetes. Whilst type II diabetes cannot be cured, individuals can have their glucose levels return to non-diabetic range (complete remission) or pre-diabetes glucose levels (partial remission). The main mechanism for achieving remission is by achieving significant weight loss. It is thought that weight loss results in increased insulin sensitivity through a reduction of inflammation, improved adipocyte function, reduced oxidate stress, reduced endoplasmic reticulum stress and improved genetic make-up. Exercise and diabetes Traditionally, exercise advice has mainly focused on aerobic activity. Aerobic exercise includes walking, running, swimming, bike riding and rowing. These exercises are of lower-intensity and can therefore be undertaken for longer periods of time, which can contribute to both lowering blood glucose and can increase energy expenditure which can aid in weight loss. However, more recently, an exercise type known as high-intensity interval training (HIIT) has shown promising benefits for acutely lowering blood glucose levels. High intensity interval training consists of short bursts of high intensity exercise interspersed with recovery periods. A common way of prescribing HIIT is known as the 4:4 method. This method involves completing 4 minutes of aerobic exercise at a low intensity which is then followed by 4 minutes of aerobic exercise at a high intensity. The intensity of exercise is alternated within this manner until a total of 16 minutes of aerobic exercise has been completed. The recommendations for achieving weight loss through aerobic exercise is to complete 300 minutes per week of moderate intensity activity, or 150 minutes per week of vigorous activity or a combination of both. In addition, exercise durations of greater than 150 minutes per week are associated with a HbA1c reduction of 0.89%, compared to those of less than 150 minutes per week which were only associated with a HbA1c reduction of 0.36%. HbA1c is a measure of your average blood glucose reading over the previous 3 months. For people with diabetes, it is recommended that the HbA1c reading is below 7%. Furthermore, resistance exercise can also have acute benefits in terms of insulin sensitivity and can increase lean body mass. Resistance exercise can also help to increase functional capacity, which can be important for those wanting to maintain independence. Meeting these recommendations are also linked to improvements in all-cause mortality, reduction in the incidence of breast / colon cancer, reduced blood pressure and improved mood, sleep, and physical function. The bottom line Ultimately, exercise plays a crucial role in the management of diabetes. Whilst diabetes cannot be reversed there are numerous benefits for those who participate in regular exercise. If people cannot meet the guidelines for exercise and diabetes there is still an abundance of health benefits that can be achieved by working towards these recommendations. Author - Rebecca Dostan References
0 Comments
In the realm of metabolic health, the adage "knowledge is power" rings especially true. As an Exercise Physiologist, Nutritionist, and Diabetes Educator, I've seen firsthand how understanding and managing blood glucose levels can significantly impact health outcomes. Continuous Glucose Monitors (CGMs) offer a powerful tool for anyone looking to optimize their health, even beyond diabetes management. Let's delve into why CGMs are beneficial for individuals with PCOS, pre-diabetes, those striving for weight loss, and women navigating menopause. Why Use a Continuous Glucose Monitor if I Don't Have Diabetes? You might wonder why a CGM would be necessary if you don't have diabetes. The answer lies in the valuable insights it provides into your body's metabolic processes. Blood glucose levels are a critical indicator of how your body responds to different foods, activities, and daily stress. By monitoring these levels continuously, you gain a real-time understanding of how lifestyle factors influence your metabolic health, allowing for more personalized and effective health interventions. The Benefits of Continuous Glucose Monitoring for Health 1. Polycystic Ovary Syndrome (PCOS) PCOS is often accompanied by insulin resistance, making blood glucose management crucial. CGMs help women with PCOS by:
2. Pre-Diabetes For individuals with pre-diabetes, CGMs are invaluable in preventing the progression to type 2 diabetes:
3. Weight Loss Weight management is intricately linked to blood glucose control. CGMs support weight loss efforts by:
4. Menopause Menopause brings about metabolic changes that can affect glucose metabolism. CGMs offer several benefits:
How Tracking Glucose Levels Results in Better Health Outcomes Tracking glucose levels with a CGM provides a clear picture of how lifestyle factors impact your metabolic health. This continuous feedback loop empowers you to make informed decisions, resulting in:
In conclusion, Continuous Glucose Monitoring is a transformative tool that extends its benefits far beyond diabetes management. For individuals with PCOS, pre-diabetes, those aiming for weight loss, and women in menopause, CGMs provide invaluable insights that drive personalized and effective health interventions. By harnessing the power of real-time glucose monitoring, you can take proactive steps towards optimizing your health and achieving better outcomes. How to access and apply a Continuous Glucose Monitor Access Our Senior Exercise Physiologist/Diabetes Educator and Nutritionist Lisa is equipped to help you access a CGM, and will support you to apply the sensor, and hook you up with a web interface and app where you can track all of your data. Not only will this track your CGM/glucose data, but you can also add in your food intake, your exercise and sleep. If you have a wearable device such as an Apple watch or Garmin, you can link the accounts and all information will be automatically transferred to give you a complete picture. How to apply a CGM Sensor - see the video below. Lisa Parkinson Accredited Exercise Physiologist Credentialled Diabetes Educator Nutritionist Diabetes management involves keeping track of various health indicators, one of which is HbA1c. But what exactly is HbA1c, and why is it important? This article will delve into the significance of HbA1c, its normal range in Australia, and how it differs from fasting glucose measurements.
What is HbA1c? HbA1c, or glycated hemoglobin, is a blood test that measures the average level of blood glucose over the past two to three months. This test is crucial for monitoring long-term glucose control in individuals with diabetes. Hemoglobin is a protein in red blood cells that carries oxygen. When glucose binds to hemoglobin, it forms glycated hemoglobin. The HbA1c test quantifies the percentage of hemoglobin that is glycated, providing an overall picture of blood glucose levels. What is a Normal HbA1c in Australia? In Australia, the target HbA1c level for most adults with diabetes is less than 7% (53 mmol/mol). However, the ideal target can vary based on individual health conditions and healthcare providers' recommendations. It's essential to have regular HbA1c tests to ensure that diabetes is well-managed and to make any necessary adjustments to treatment plans. What Does the HbA1c Mean? The HbA1c level reflects the average blood glucose concentration over the past two to three months. Here's a breakdown of what different HbA1c levels indicate:
Regular monitoring of HbA1c helps to assess how well diabetes is being managed and to identify any necessary changes in treatment to prevent complications. What is the Difference Between Fasting Glucose and HbA1c? Fasting glucose and HbA1c are both important measures in diabetes management, but they serve different purposes:
Both tests are essential: fasting glucose can identify acute spikes in blood glucose, while HbA1c offers a broader view of how well blood glucose is controlled over time. Need more info? For more detailed information on managing diabetes and how your Exercise Physiologist can help, please refer to the following resources:
Take Action Taking control of your diabetes is crucial for long-term health. Regular monitoring and appropriate lifestyle changes can make a significant difference. Book an appointment with our experts to develop a personalized diabetes management plan. Book Now Conclusion Understanding HbA1c and its role in diabetes management is vital for maintaining good health. Regular HbA1c testing, alongside fasting glucose tests, provides a comprehensive view of your blood glucose control. By staying informed and proactive, you can effectively manage your diabetes and enhance your quality of life. Why Men’s Health? In Australia, the conversation around men's health has gained significant traction in recent years. The World Health Organization (WHO) defines health as 'a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity'. For men, the three most common causes of ill health and disease burden are cancer, cardiovascular disease, and mental health issues. As we delve deeper into the statistics and realities, it becomes evident that proactive measures are crucial in promoting overall well-being among men. The majority (79%) of illnesses and diseases affecting males are modifiable through exercise and other healthier habits. Furthermore, men's total burden of disease is 1.2 times that of women, reflecting its economic and societal impacts on the population (2). This underscores the growing support for the use of exercise and lifestyle adjustments in maintaining optimal health. These statistics clearly position men’s health squarely within the scope of the WHO definition and emphasize its importance as a focal point for exercise physiologists.  Correlation of fitness to threshold for dependence (7) The role of exercise Exercise is not merely about physical fitness but is integral to maintaining mental well-being. Regular physical activity has been shown to reduce the risk of chronic diseases such as heart disease and diabetes, while also improving mood and reducing stress levels. Initiatives promoting active lifestyles among men have seen encouraging results, emphasizing the positive impact of exercise on overall health. Men who have increased aerobic fitness and muscular strength have improved other aspects of wellness such as dietary habits, lesser consumed alcohol, increased steps daily and consistency with dental health just to name a few (4). What types of exercise you may ask? 1. Cardiovascular Exercise: Activities such as brisk walking, jogging, cycling, or swimming help improve heart health and boost overall endurance. Recently high intensity interval training or HIIT has become popular and it stands as a sound choice recently demonstrating with both short and long rest periods a noteworthy improvement in VO2Max comparatively to other methods of training (5). 2. Strength Training: Incorporating resistance exercises with weights or body weight (e.g., push-ups, squats) builds muscle strength and supports bone health. Men particularly respond well in health outcomes and quality of life scores with an increase intensity of exercise versus women, so try find yourself some big weights for your exercises (6). 3. Flexibility and Balance: Practices like yoga or tai chi enhance flexibility, balance, and coordination, reducing the risk of falls and injuries. Lifestyle Changes for Better Health Beyond exercise, lifestyle choices play a pivotal role in men's health. Dietary habits, smoking, and alcohol consumption are critical factors influencing overall well-being. Embracing a balanced diet rich in fruits, vegetables, and lean proteins supports physical health, while reducing tobacco and alcohol intake can mitigate the risk of chronic diseases. Australian businesses are stepping up to promote healthier lifestyles among employees, offering wellness programs that educate and incentivize positive choices. By fostering a culture of health within workplaces, organizations contribute not only to the individual well-being of their employees but also to increased productivity and morale. This could be the beginning of your changes if you think of how much of your time you spend at work in a week. Recommendations for Lifestyle Changes: 1. Healthy Eating: Opt for a diet rich in fruits, vegetables, whole grains, and lean proteins while minimizing processed foods and sugars. A good place to start is following the Australian Guide to Healthy Eating, or even visiting a dietitian if you are particularly stuck.  Australian Guide to Healthy Eating (1) 2. Smoking Cessation: Seek support through smoking cessation programs and resources to quit smoking for good. Your doctor, Exercise Physiologist and other health professionals can always refer you to the right place.
3. Moderate Alcohol Consumption: Limit alcohol intake to reduce the risk of liver disease, cardiovascular problems, and mental health issues. Again there are guidelines out there (eg. No more than 10 a week, or 4 in a day) but if you need support always consider your doctor as an ally. Seeking Professional Guidance For men looking to kickstart their journey towards better health, consulting an exercise physiologist can be highly beneficial. These specialists are trained to assess individual fitness levels, tailor exercise programs, and provide guidance on achieving health goals effectively and safely. Whether recovering from an injury, managing a chronic condition, or simply aiming to improve overall fitness, an exercise physiologist offers personalized support and accountability in optimizing health outcomes. Addressing men's health in Australia demands a collective effort to promote exercise and lifestyle changes. By raising awareness, advocating for preventative measures, and supporting healthy choices, we can empower men across the country to lead fulfilling and healthy lives. Together, we can build a future where men's health is prioritized, ensuring a stronger, healthier Australia for generations to come. Thomas Harrison Resources used for further reading:
What is lower back pain? Lower back pain is an extremely common presentation, as it is estimated that up to 70% of individuals will experience lower back pain within their lifetime. Lower back pain can have various underlying causes. Yet, it is reported that up to 85% of all cases have mechanisms that are poorly understood. Consequently, this results in this type of back pain being classified as non-specific (or having an unknown origin). However, there is evidence to suggest that exercise can play a vital role in reducing symptoms. Exercise can improve back strength, flexibility, and range of motion.1 Exercise can also help to improve function and mood and ultimately promote good health. Below are 4 exercises that you can complete at home, which can help reduce symptoms of lower back pain and provide relief. Knee to chest stretch For this exercise, lie down on your back (your bed or a firm couch is a great place for this exercise). Start by slowly bringing one knee towards your chest. You should feel a gentle stretch within your glutes and hamstrings. Try holding this stretch for 10 seconds. Importantly, with stretching you should not stretch to the point of pain. That is, stretching should be pain free. Once you have held this stretch for 10 seconds, alternate to your opposite side holding for 10 seconds. Pelvic tilts The next exercise that you can try is a pelvic tilt. Lie down on your back with your knees bent and feet flat on the floor. Next try to flatten your lower back down onto the ground. You can do this by trying to pull your bellybutton towards your spine and squeezing your glute muscles. You should feel the majority of effort occurring with your abdominal and glute musculature. You can start by completing 2 x 10 repetitions. Bridges This exercise is known as bridging or bridges. Again, lie down on your back with your knees bent and your feet flat on the floor. Perform a pelvic tilt and then lift your hips up off the floor. Try to lift your hips up to a height where a straight line is made through your knees, hips, and shoulders. Then, slowly lower your hips back down to the starting position. You can start by completing 2 x 10 repetitions for this exercise also. Deadlift To start this exercise, you want to position the bar above the balls of your feet and have your feet approximately shoulder width apart. Squat down to pick up the bar using an overhand grip. Once standing upright stand with your knees slightly bend. Hinge forward with your hips and keep your back straight (like you are taking a bow) whilst running the bar along your legs. Squeeze your glutes and hamstrings to return to the starting position. You can start by completing 2 x 8 for this exercise. When selecting a weight, make sure you feel as though you could still complete an additional 3 – 4 repetitions once you have completed 8. Ultimately, being active and making sure we move can help improve symptoms of lower back pain over the long term. 2 The key is finding an exercise or an exercise routine that works best for you. If you would like further information, feel free to consult your local accredited exercise physiologist.
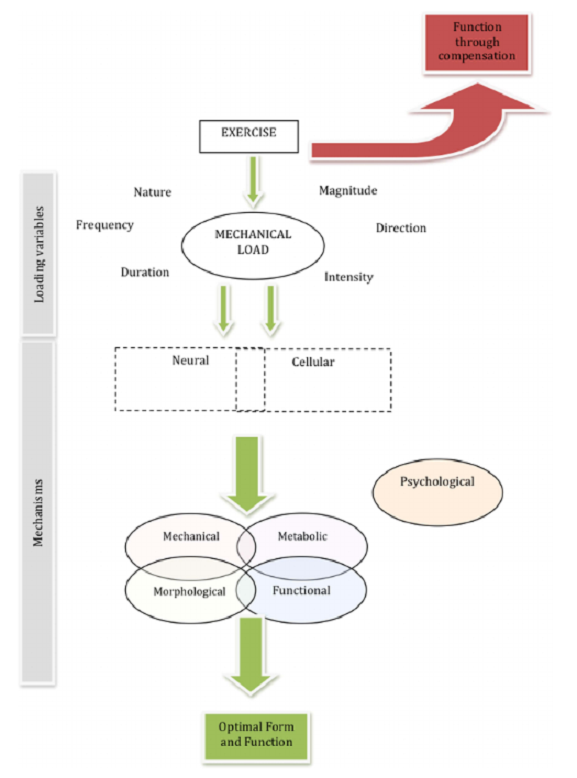
References Searle, A, Spink, M, Ho, A & Chuter, V 2015, ‘Exercise interventions for the treatment of chronic low back pain: a systematic review and meta-analysis of randomised controlled trials’, Clinical Rehabilitation, vol. 29, no. 12, pp. 1155–1167. Exercise is Medicine 2024, Exercising with lower back pain, Exercise is Medicine, viewed 30 May 2024, <EIM Rx series_Exercising with Lower Back Pain.pdf (exerciseismedicine.org)>. What is aerobic fitness? Aerobic fitness can be defined as one’s ability to transport and deliver oxygen to the muscles, so it can be utilised to generate energy to support the activity of the muscle during exercise (1) There are three major components to aerobic fitness which can be viewed below (2).
General exercise recommendations for increasing your aerobic fitness 3
Training methods for increasing your aerobic fitness. There are three basic forms of aerobic fitness training: continuous training, interval training and Fartlek training (4). Continuous training Involves continuous exercise such as jogging, swimming, walking, or cycling, at “somewhat hard to hard” intensities without rest intervals. The prescribed exercise intensity is maintained consistently throughout the exercise session. Interval / HIIT training
Fartlek training Fartlek training or “speed play” is similar to interval training, but is a free form of training, which involves interspersing short bursts of intense/faster work throughout a continuous training activity. The exercise-rest cycle is not systematic or precisely timed and measured but is based on the feelings of the participant. The bottom line
Completing some form of aerobic exercise is better than completing no aerobic exercise. If you’re not sure where to start, it is best to start with small increments (5 – 10 mins) of light intensity exercise (walking or cycling) and slowly increase the duration over time. Once you can comfortability tolerant this, look to start increasing the duration. Once you can complete greater bouts of aerobic exercise look to increase the intensity, eventually aiming to reach the recommended guidelines. Bec Dostan
As women enter the transformative phase of menopause, they often find themselves grappling with unexpected health challenges. One significant aspect that deserves attention is the connection between menopause and insulin resistance, is this causing excess weight gain, especially around the tummy? Let's explore insulin resistance during this time. What is insulin resistance? Insulin resistance or impaired insulin sensitivity is when the body becomes intolerant to insulin, making the hormone less effective. Insulin is often said to be like a key in the body, unlocking doors, and insulin resistance is like having dud keys! What is Insulin’s role in the body? Insulin is an important hormone within the body as it helps the body to use glucose for energy. When foods containing carbohydrates are consumed, they are broken down by the body into glucose and released into the bloodstream. The hormone insulin is signalled to be released by the beta cells of the pancreas, enters the bloodstream, and helps glucose to move out of the blood and into the cells/tissues of the liver, muscle, and adipose tissue where it can be used for energy later on (insulin is like the key that opens the cell doors and allows glucose to enter).5 In addition to helping regulate blood glucose levels, insulin also plays a part in other essential processes within the body including the synthesis of lipids and regulation of enzymatic activity. What causes Insulin Resistance The factors that promote the development of insulin resistance include altered insulin signalling, high levels of insulin in the body, high lipid (fat) levels in the body, and obesity.2 There are several risk factors for insulin resistance, these being if you:
How is Insulin Resistance Diagnosed Generally, individuals do not show any symptoms of insulin resistance. If your GP believes that you are at risk of insulin resistance, they may request a blood test to investigate further. How does Insulin Resistance relate to menopause? Research has shown that menopause is a potential risk factor for developing insulin resistance, regardless of age, and most likely due to the reduction in estrogen in the body. Some clinical studies have shown that post-menopausal women are more susceptible to developing dyslipidaemia (high lipid levels), an increase in body weight (assessed by Body Mass Index and waist circumference), and impaired glucose tolerance than premenopausal women.8 Even in the absence of a change in body weight, cross-sectional studies indicate that as women approach postmenopause, their abdomen fat increases. The drop in estrogen, which instructs fat to be stored in the hips and thighs, is connected to this rise in the deposition of belly fat. Visceral (between the visceral organs) and subcutaneous (under the skin) fat are two types of abdominal fat. Because visceral abdominal obesity is also linked to dyslipidaemia, insulin resistance, and hypertension, it independently increases the risk for cardiovascular disease (CVD).10 Estrogen replacement therapy has been shown to significantly reduce the risk of metabolic syndrome, in contrast to metabolic disturbances, such as insulin resistance, tending to increase with the onset of menopause.2 It has therefore been summarized that estrogen plays a protective role in the development of insulin resistance and its related health effects. What can you do to improve insulin resistance? Several risk factors for metabolic syndrome and insulin resistance are lifestyle-related, including a high sugar intake, a high-fat diet, being overweight or obese, and being physically inactive. These are controllable risk factors, and a healthy lifestyle can have a positive impact on these, including reduced insulin resistance. Weight Management Significant improvements in insulin sensitivity can be achieved through weight reduction in the overweight and obese population. Adaptations that occur with a combination of improved nutrition and exercise are the most effective methods in achieving sustainable weight loss and improvements to insulin resistance.7 Nutrition Carbohydrates are crucial to the body and are our main form of energy, however, inappropriate intake of carbohydrates can lead to poor health outcomes. Guidelines informing nutritional changes and recommendations for the dietary management of insulin resistance are to:
If you have been diagnosed with insulin resistance, an Accredited Practicing Dietitian is the right person to guide you with a nutrition program suitable to your needs. Exercise As stated above, exercise can form part of a weight loss program if needed, however, the benefits of exercise to insulin sensitivity and reduced insulin resistance are independent of weight loss:- meaning that you can achieve improvements in insulin resistance by exercise alone 8. In addition to improving insulin resistance, females can also experience the following through regular exercise:
A systemized review in 2017 examining the effect of programmed exercise on insulin sensitivity in postmenopausal women found that regular exercising for 3 to 4 months significantly lowered insulin levels, body mass index, waist circumference, and percentage body fat mass in postmenopausal women.1 How much and what type of exercise? The Australian Physical Activity Guidelines recommend that individuals undertake a minimum of 150 minutes of moderate-intensity cardiovascular exercise (5 days or more per week of 30 to 60 minutes) or 75 minutes of vigorous-intensity cardiovascular each week, in addition to 2 resistance training sessions weekly (on non-consecutive days). This is the absolute minimum amount recommended, with greater improvements in insulin resistance, weight reduction, and reduction in risk of death from cardiac conditions being obtained with increased levels of cardiovascular exercise up to 300 minutes/week (of moderate-intensity cardiovascular exercise.) 4 Research has shown that regular exercisers who demonstrate high levels of physical activity exhibit high levels of insulin sensitivity/insulin action. If these exercisers then cease exercise training, they then show a decrease in insulin action, demonstrating that regular exercise is required to sustain improvements in insulin sensitivity. 7 All forms of exercise training including aerobic, interval, and resistance training, with or without body composition changes/weight loss have been shown to improve insulin sensitivity and metabolic syndrome factors such as HDL cholesterol, triglycerides, blood glucose and blood pressure, cancer risk, type 2 diabetes risk and cardiovascular disease risk reduction.9 And, even in females whose insulin sensitivity was found to be reduced in early post menopause, following 3 months of high-intensity exercise training, they were able to increase their peripheral insulin sensitivity, skeletal muscle insulin-stimulated glucose uptake, and skeletal muscle mass to the same extent as premenopausal women.8 What are forms of cardiovascular exercise?
What is resistance training? Resistance training is when a limb is moved through a range of movement against resistance. This may include initially using body weight (such as a squat) and progressing to using heavier resistances such as dumbbells, kettlebells, barbells, and resistance machines. Exercise of our skeletal muscles should occur at every stage of life, but after menopause, resistance training becomes even more crucial for women because of the quick reduction in bone density, muscle mass, and joint health that occurs as women age. GETTING HELP An optimal exercise prescription should be individualised and prescribed by an Accredited Exercise Physiologist (AEP) following a complete health screening and assessment by the AEP. The exercise program will then be tailored to the individual and include aerobic training and resistance training, in addition to balance and pelvic floor training if appropriate. Lisa Parkinson Accredited Exercise Physiologist and Credentialed Diabetes Educator References
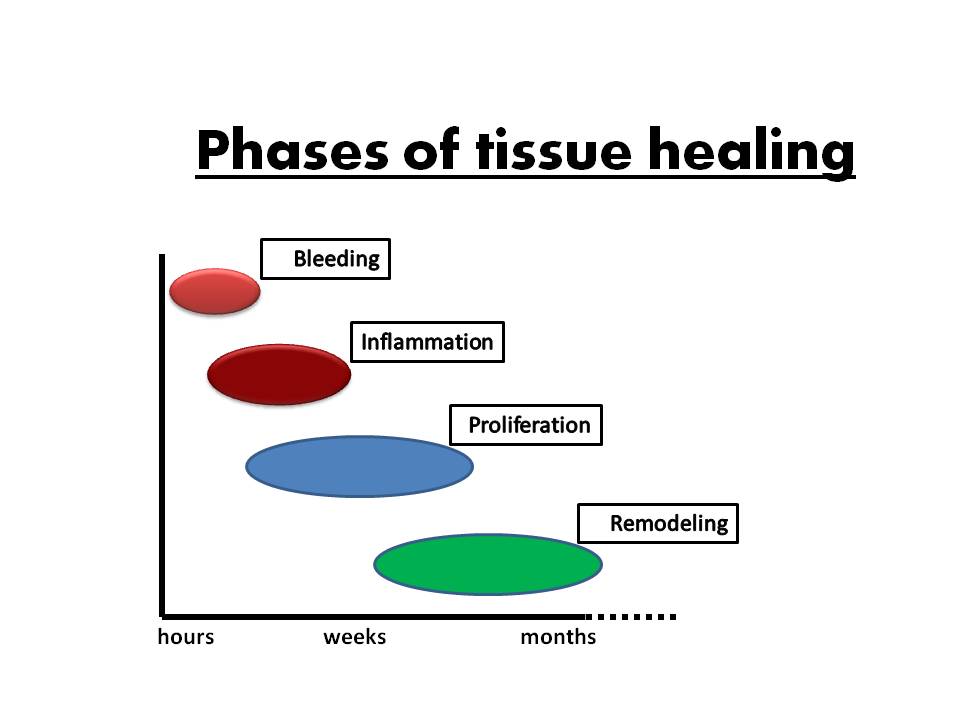
In 1978, Gabe Mirkin a now renowned scientist in the health and wellness space, coined the phrase RICE regarding an approach to injuries. This being Rest, Ice, Elevation, and Compression. For years this has been the gold standard immediate response to an injury of a joint or a muscle and you may have heard the phrase because of how widespread it has become. I want to ask you though; Have you heard of PEACE & LOVE? This one stands for Protect, Elevate, Avoid analgesics, Compression, Educate, Load, Optimism, Vascularisation and Exercise. In 2015 Gabe Mirkin released an official report no longer standing by the previously popular RICER tool. Increasingly active recovery becoming a more evidence-based approach to injury first aid. Active recovery and loading are how you should approach a new injury to get you back to doing the activities you love sooner! Before I can get to this, let me point out to you why rest isn’t the best course of action, then I can tell you why exercise is the best. Without getting too ‘science-y’; although if you were to aggressively load the joint or immediately protect the injury, prolonged rest can lead to undesirable modification or mechanics through the healing process. Think about the reasons for why we prescribe exercises for you in a clinical setting if you’re looking to rehabilitate a muscle or joint. The load and stress induce a response from the body to improve tissue redevelopment. A great anecdote for this approach of shortened rest is, following hip or knee replacements you’ll see people getting discharged from hospitals as soon as they can manage a flight of stairs. When you injure a muscle, bone or any other component of a joint, inflammation is a necessary stage in the healing process. Ice acts inversely to the natural inflammation process. While ice can be an effective short-term relief for pain resulting from the injury, it will narrow blood vessels, stunt flow of hormones and immune factors and then continue to slow this necessary inflammation. Check out the process here ↓ In the same category as ice are other analgesics such as steroids, NSAIDS and immune suppressants, to name a few. It is important to note that anything that reduces inflammation will result in delayed healing. The other components of the RICE protocol that remain in the PEACE & LOVE protocol are Compression and Elevation. Both have many clinical applications and the principles of using these lies in venous return and aiding flow of blood and immunogens. Although there is competing data for efficacy of these tools, there is no evidence that these slow the healing process and they remain in the best practice initial response to injury. Let’s give ourselves PEACE! The LOVE in the new acronym represents the prescription you would receive in a rehabilitation program and the changes that occur in the body due to this. I’ve included a graphic which visualises what we’d prescribe in a program versus what happens if it is left alone, or simply put: rested. Within a well prescribed exercise program there will be changes in your ability to load, positivity associated with moving and your aerobic and cardiovascular capacity. These things forming the final portion of LOVE, being Load, Optimism, Vascularisation and Exercise. So please following an injury show yourself some LOVE and see a professional! Furthermore, from these changes in best practice from the last decade there are extra approaches and research being undertaken. Another study ongoing from Campbell in 2013 is MEAT (Movement, Exercise, Analgesia, & Treatment) or Robinson in 2017 is MOVE (Movement, Options, Vary, Ease). These both examining active recovery rather than rest showing increasingly more evidence for exercise versus rest. I’ll leave you with one more tool to consider from Reinl in 2013 being ARITA, meaning ‘active recovery is the answer’. Hopefully you take this approach next time you have an injury occur. Thomas Harrison
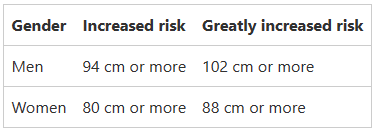
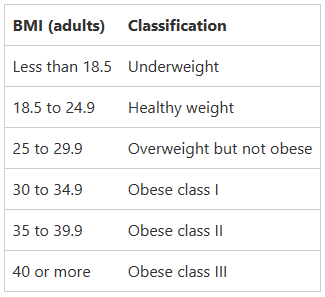
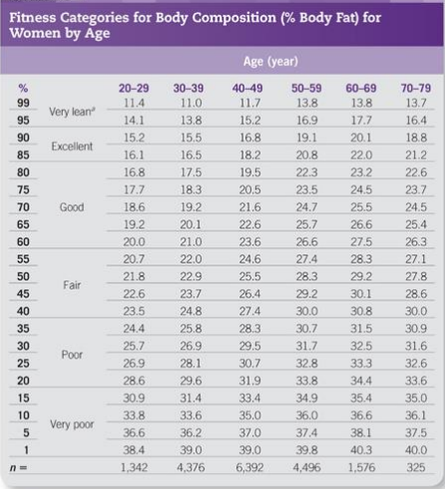
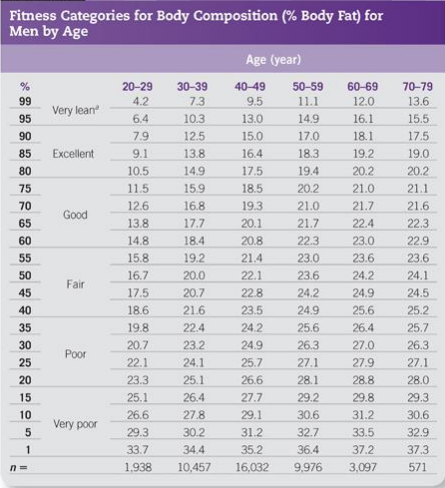
Accredited Exercise Physiologist In Australia 67% of adults are overweight according to the AIHW, the Australian Government agency for health and welfare data. To repeat the significance in this statement, that is 2 out of 3 adults in Australia who have a BMI classed as overweight or obese. This factor alone has in the last decade been ranked as the number one cause of disease burden in Australia. Not only that the World Health Organisation has estimated that of all non-communicable diseases those related to overweight and obese populations make up around 90% of Australia’s deaths annually. If these aren’t immediately significant enough for you, I want to outline within this write up the importance of all the measurements you complete with an Exercise Physiologist and other health professionals, and a summary of some of the changes you can make to positively affect your physical health and wellbeing. What are the measurements you will have taken by an Exercise Physiologist? Body Mass “The weight of a person or thing is how heavy they are, measured in units such as kilograms, pounds, or tons.” BMI “Body Mass Index is a measure of body fat, that is the ratio of the weight of the body in kilograms to the square of its height in metres.” Body Composition “The different components (or "compartments") of a human body. The selection of compartments varies by model but may include fat, bone, water, and muscle.” Waist Circumference “The measurement around the narrowest point of the abdomen, or the midpoint between the lower border of the rib cage and the iliac crest. Used as an indicator for abdominal obesity.” What are the outcomes of each of these measurements? Body mass and BMI go hand in hand and as you can imagine, as the weight increases or decreases so does the number in the BMI score. The current trend for Australians is that we each gain an average of 300grams to 500grams with every year. Those increases yearly align with the rapid increases we’ve seen in our country the last 2 decades of overweight and obese individuals, again these have seen an increase of between 14% to 27% across different age brackets as recorded by AIHW. Having an overweight or obese BMI attributes to 30 diseases, including 17 types of cancers, 4 cardiovascular diseases, 3 musculoskeletal conditions, type 2 diabetes, dementia, asthma and chronic kidney disease. Here is a table of the classes of BMI for reference, with the healthy range being <25kg/m2. When recording body composition in our clinic the results measured include fat mass (both total fat mass and visceral fat), muscle mass, bone density, and body water to name a few. If your goal is weight loss than the figure you want to decrease is your fat mass. The other components such as muscle mass, bone density and body water can help flag and monitor other conditions such as osteoporosis, muscular atrophy, and more. When considering body fat here is a representation of what ranges are considered healthy: Within this component, there is increasingly more evidence supporting that the visceral body fat represents higher risks of cardiovascular and metabolic risks. This is the fat that is deposited around the organs. Independent of otherwise healthy organs, visceral body fat continues to present cardiovascular risk and metabolic risk when it makes up for >10% of the total body fat count. Here’s a guide on where these numbers should sit on the scale 0-59: When measuring waist circumference, the aim is to guide health professionals on risk levels associated with abdominal fat and total body fat that may be increased. The evidence surrounding measuring waist circumference for these risks is increasingly more valid for quantifying health risks; the current guidelines for these are below: In the previous decade in Australia, the trend for our waist circumference as we age is accelerating by 0.42cm every year, not dissimilar to the increase in weight discussed earlier. This makes for a compelling correlation. When looking at reliability of these measures, waist measurements applied with other data such as waist to hip ratio, waist to height ratio or coupled with a BMI score, these demonstrate a good strength of correlation coefficient of at least 0.82 across the board. The correlation being how strongly linked the result is to cardiovascular and metabolic risk factors, and scored from -1.00 to +1.00. What can be done to reduce your risk of illness if you are outside these healthy ranges?
At the risk of repeating everything you’ve heard from your doctors, family, friends, or out in society; increase your physical activity and change some of your eating habits. Specifically try meet these guidelines:
Thomas Harrison Accredited Exercise Physiolgist With age comes more wisdom, knowledge and experience! But unfortunately, pain also increases with age. 1 in 5 (20%) people aged 65–74 reported having chronic pain, increasing to 22% of those aged 75–84 and 24% of those 85 and over. I truly believe knowledge is power and with changes in understanding around persistent pain let's have that understanding widespread. That is what the purpose of this blog is, to help the older and wiser population understand pain and how we can help. It's Like an Alarm on Your Car Persistent pain management has progressed immensely over the last 10-15 years. From a completely biomedical approach (I hurt because the body tissues are damaged) to a more contemporary model based on the most recent research that tells us that pain is a protection mechanism for the body to prevent injury or damage. In simple terms, pain is the alarm system of the body, it gives us a protective buffer and reminds us not to do too much too soon. It is a safeguard to keep our body and its tissues safe. It is a normal response to potential danger and is always 100% real! What do I mean? Ever reversed your car into a pole? Before you hit the pole, the car beeps at you and warns you of the danger behind you. Well, this is like pain. As you get closer to the pole the car beeps faster and faster and eventually if you ignore it, you hit the pole and injure the car (ouch). Once injured, the sensitivity of this alarm goes up, things that might not have hurt before, do and things that would only hurt a little, hurt a lot. This is for protection and to promote healing. Usually, as the body heals the sensitivity decreases and everything goes back to normal. Think of being sunburned and getting in a hot shower. That burns doesn't it? But once the body heals from sunburn that same shower doesn't hurt anymore. The overprotective Alarm Now you have a grip on why pain is needed. Let's dive into when it hangs around! This is caused by an over-sensitive pain system. What this means is that the pain system that had increased its sensitivity due to an injury has not returned to normal, even though normal healing has taken place, pain has continued. This is unhelpful and prevents recovery. Think of the beeping car. The car beeps faster and louder even though you aren't in danger of hitting the pole. Unfortunately, I can't answer why the pain system may stay in overprotective mode but there are some things I can tell you:
How does exercising turn the alarm down? We here at Optimum EP advocate strongly for exercise because we know the huge amount of benefit someone can see in all aspects of their health. And you guessed it, Exercise can be a helpful mechanism for perisitent pain also. This proces is called exercise hypoalgesia which simply means engaging in exercise can help alleviate or decrease painful symptoms. This happen several different ways including:
Now disclaimer incoming: Exercise may not completely alleviate pain, BUT it can significantly improve pain management, reduce the need for pain medications, and enhance overall well-being. Haven’t convinced you yet? Now if you are struggling with the idea of exercise for pain management let me indulge in a little advocating. Exercise is the most powerful intervention in which can simultaneously help management huge range of different chronic conditions and give you a enormous amount of benefit in one action. “If exercise was made into a pill, it would be the most prescribed pill in the world.” Read that one again. Exercise is so powerful in some cases research has shown it to out-perform medication. And guess what, it is all natural, anyone can do it and it is free. Now I am going to list 10 different ways exercise can help you aside from pain management:
Tips for starting! The key to successfully starting an exercise program with persistent pain is to:
The journey is unique for each person, so there's no need to rush. In fact, taking the time to build a solid foundation is often the path to long-term success. Seek the guidance of one of our Accredited Exercise Physiologist to tailor your exercise plan to your specific needs and limitations. Remember, the most important thing is to start, keep moving forward at your own pace, and celebrate the small victories along the way. Izaac Boylan Accredited Exercise Physiologist |
AuthorSLisa Parkinson Archives
July 2024
Categories
All
|















 RSS Feed
RSS Feed